If you followed Media MICE’s coverage of the World Ophthalmology Congress (WOC2020 Virtual), you may recall some of the conditions we highlighted during the event. A national anti-cataract project in Ghana stood out, as did the treatment of ocular trauma in countries like Somalia where resources are limited. Another condition we focused attention on was ocular syphilis.
We wrote at the time that ocular syphilis is not everyone’s “favorite medical malady,” but to be sure, it is a fascinating condition. Syphilis is insidious, diffuse and complex with a variety of symptoms and various stages of development. While it is, of course, most widely known in the lay community for its association with sexual contact, to ophthalmologists, it is most interesting because of a complication known as ocular syphilis.
Ocular syphilis is usually associated with the tertiary or late stage form of syphilis, with onset of three to 15 years post-infection; however, it may occur at any stage of the syphilitic process. Ocular syphilis can involve almost any eye structure, with posterior uveitis and panuveitis being the most common. However, additional manifestations may include anterior uveitis, optic neuropathy, retinal vasculitis and interstitial keratitis.1 Ocular syphilis may lead to decreased visual acuity — including permanent blindness — and is most associated with neurosyphilis, the infection of the central nervous system.
Syphilis Can Literally Rot Your Skull Away
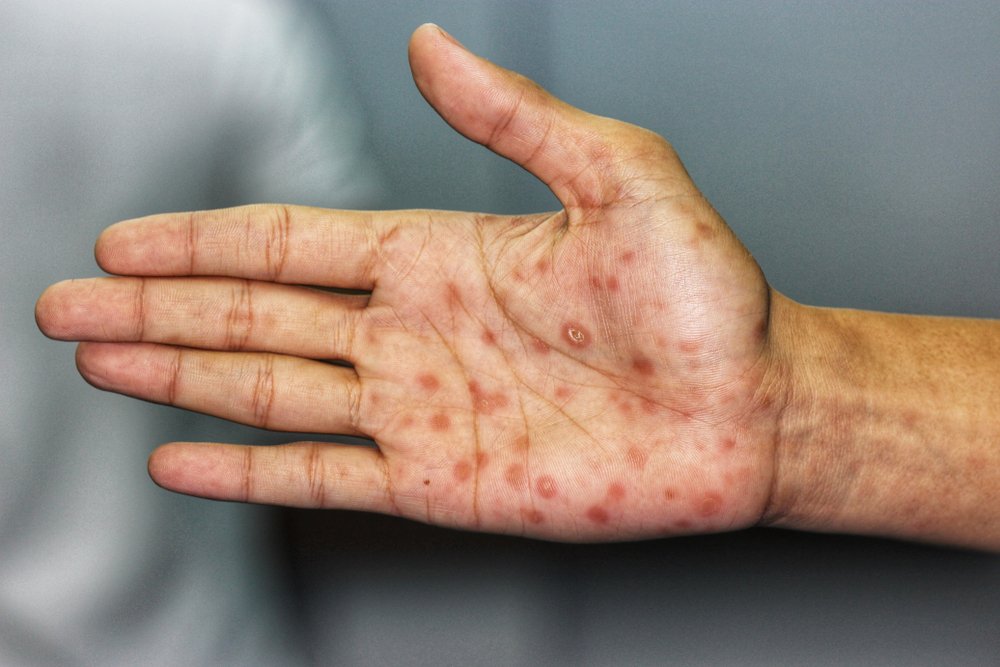
Our reporting on ocular syphilis during WOC2020 Virtual focused on its frequent presentation concomitant with human immunodeficiency virus (HIV), a common problem in Africa. One study carried out by researchers from Stellenbosch University and Tygerberg Hospital in Cape Town, South Africa, reported that 52.1% of patients with ocular syphilis also had HIV.2 Similar findings have been reported in countries as varied as Ethiopia, Malaysia and China.
The diagnosis of ocular syphilis in and of itself can be challenging due to lack of pathognomonic findings. This difficulty spurred a group of researchers in Shanghai, China to describe risk factors for ocular syphilis and clinical features of blindness. The study examined patients at the Shanghai Skin Disease Hospital; in the study, there were 8,310 new cases of syphilis, of which 213 had ocular disease and 50 were blind due to syphilis.
The authors found that blindness from syphilis was restricted predominantly to patients with optic nerve involvement and not patients with isolated uveitis. At last follow‐up, vision had improved in 24 of 67 eyes (35.8%) after treatment. The conclusion was that early recognition and diagnosis is vital to avoid permanent visual loss.3
Pandemics and the Pox Return

However, before you start to believe that this is a problem of the developing world alone, think again. Over the last decade rates of syphilis have been rising in the developed world too, and it is rapidly becoming a silent public health crisis. As rates of syphilis infection increase in the Westen world, so too do rates of ocular syphilis.
Take France, for example: The country has one of the highest rates of syphilis infection in Europe and the situation is worsening every year. This is driven by unsafe sex practices among men who have sex with men (MSM), with nearly two thirds (62%) of reported transmissions.. In one study, 21 cases of ocular syphilis were reported between 2012 and 2015 at a tertiary reference center in Paris, France.4
The occurrence of ocular syphilis increased from 1 case in 2012 to 5 cases in 2013; 6 cases in 2014; and 9 cases in 2015 (2.22–25.21/1,000 individual patients/year for the period). Among these cases, an annual 20 to 33% were co-infected with HIV. This study highlights both the growth in ocular syphilis in one country, while following a familiar pattern of association with HIV.
These findings concur with another study into ocular syphilis in North Carolina, which examined 7,123 patients living with syphilis. Of these cases, 2,846 (39.9%) were living with HIV, 109 (1.5%) had ocular syphilis and 59 (0.8%) had both, with ocular syphilis being more prevalent in patients with HIV compared to HIV-negative/unknown-status patients. The study went on to conclude that HIV-related immunodeficiency possibly increases the risk of ocular syphilis development in co-infected patients.5
So what conclusions can we draw about the increasing rates of ocular syphilis? For clinicians, it is recommended to screen for syphilis and especially ocular syphilis in patients who are HIV positive. For the general public, especially MSM individuals in developed countries, increasing measures to ensure safer sex via protection should be taken.
References
- Clinical Advisory: Ocular Syphilis in the United States. Centers for Disease Control and Prevention. Available at: https://www.cdc.gov/std/syphilis/clinicaladvisoryos2015.htm. Accessed on January 27, 2021.
- 2. Matthew D, Smit D. Clinical and laboratory characteristics of ocular syphilis and neurosyphilis among individuals with and without HIV infection. Br J Ophthalmol. 2021;105(1):70-74.
- Gu X, Gao Y, Yan Y, et al. The importance of proper and prompt treatment of ocular syphilis: a lesson from permanent vision loss in 52 eyes. J Eur Acad Dermatol Venereol. 2020;34(7):1569-1578.
- Pratas AC, Goldschmidt P, Lebeaux D, et al. Increase in Ocular Syphilis Cases at Ophthalmologic Reference Center, France, 2012-2015. Emerg Infect Dis. 2018;24(2):193-200.
- Cope AB, Mobley VL, Oliver SE, et al. Ocular Syphilis and Human Immunodeficiency Virus Coinfection Among Syphilis Patients in North Carolina, 2014-2016. Sex Transm Dis. 2019;46(2):80-85.



